Thepatientisintheroom.Thedoctorisinthechart.
Twenty years of electronic health records have produced the best-charted, most burned-out physician workforce in history. We think the next generation of clinical software should let doctors practice medicine instead of typing about it.
The problem
The chart became the patient.
We built systems to satisfy billers, regulators, and lawyers, and we asked physicians to operate them in real time, in front of sick people. The result is the most documented, least present medicine in human history.
Every clinical encounter now has three participants: the patient, the physician, and the chart. Two of them are losing.
We do not blame any one vendor. We blame the premise that a record-of-care system should also be the system of action, the system of billing, the system of compliance, and the user interface for medicine itself.
That premise has reached its ceiling. Adding another tab will not fix it.
A typical day
The EHR day, in three numbers.
Most happen in front of the patient.
While the patient is still talking.
After everyone else has gone home.
Day shift · per encounter
Mouse-clicks during a typical 10-hour shift.
Most happen between you and the patient. The chart wins the room.
Of every clinic hour
is spent in the EHR and on desk work.
Time at the bedside has been crowded out by the screen at the bedside.
After clinic ends
of “Pajama time” documenting at home.
Care no longer ends when the door closes.
Try it · 60 seconds
Write one note. Count the clicks.
Below is a small simulation of one outpatient note in a typical EHR. Not a satire, just compressed. Open it. Try to finish.

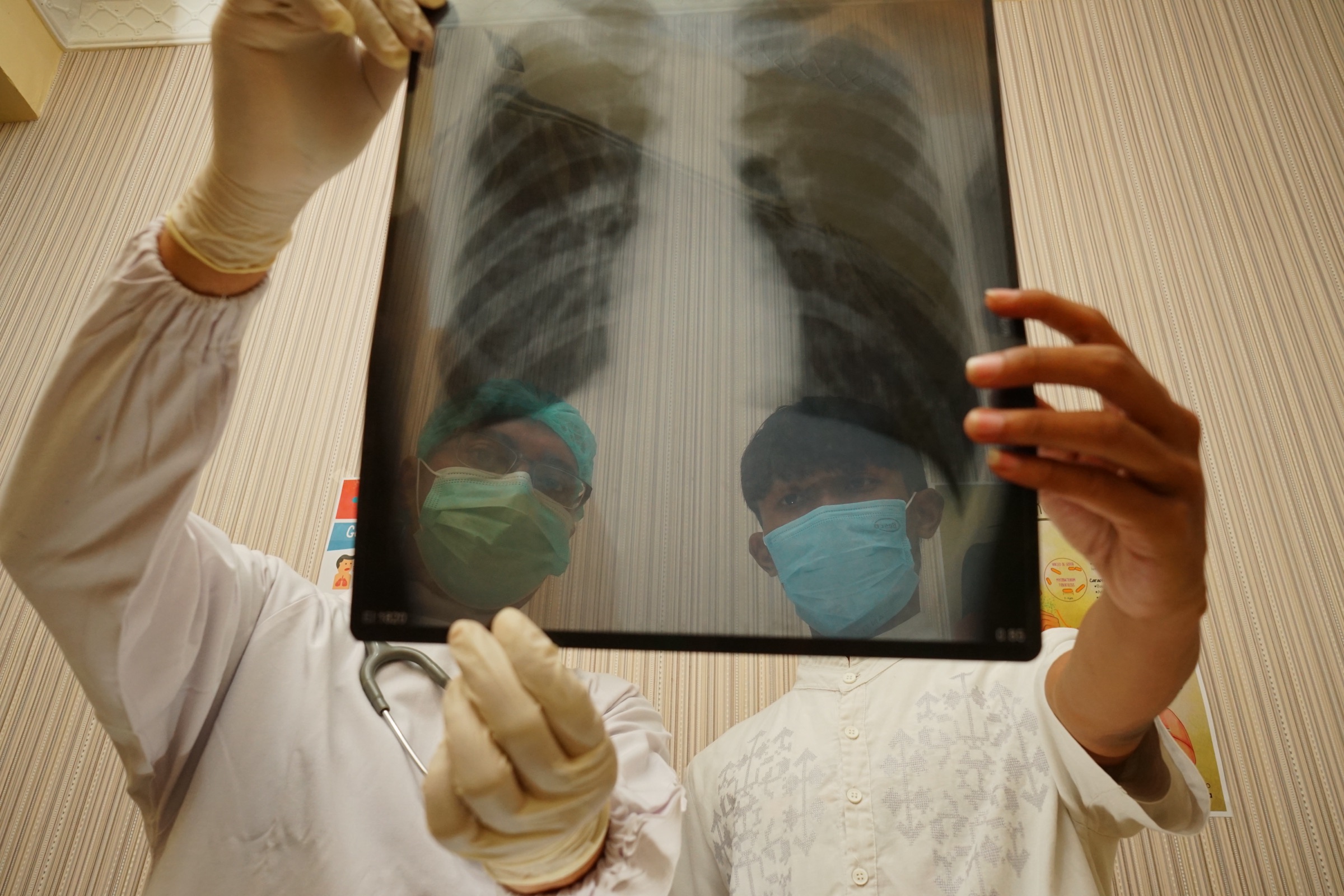
The doctor used to be the instrument. Now the image is.
Then: a physician at a child’s bedside. Now: clinicians at a film of the lungs — the patient is somewhere else.
Joseph Tomanek, after Luke Fildes, c. 1933 (after 1891 original) · M. Joko Apriyo Putro, 2023
What we lost
Medicine used to be a conversation.
A history. A look. A hand on the abdomen. Then a thought, then a plan, then a few words in a chart at the end of the day. The chart was a record of the work, not its substitute.
Eye contact
The first diagnostic instrument. Now competing with a screen for attention.
Continuity
The story of a patient, told by the people who care for them — not auto-populated from yesterday’s template.
Time
The substance physicians actually deliver. Currently spent on data entry.
On the other side of the screen
What physicians actually say.
Anonymized so they can speak honestly. Lightly edited for length only.
“My daughter learned the phrase “after Mommy finishes her notes.” She is four.”
Family medicine — Midwest, U.S. “I went into medicine to look people in the eye. I spend my day looking at a screen with my patient out of focus behind it.”
Internal medicine — Northeast, U.S. “There is a click for everything. Including a click that asks me if I am sure I want to click.”
Emergency medicine — academic center “The chart is the patient now. We are doing medicine for the chart.”
Hospitalist — community hospital
A different premise
Software should do the typing.
Modern systems can listen, retrieve, reason, and act. Used carefully, they can take on on the work that has been parasitizing clinical attention for two decades — documentation, ordering, billing, prior auth, follow-up — and leave the physician with the only things only a physician can do.
We do not mean another sidebar. We do not mean another “assistant” that asks for your password. We mean systems that perform finished tasks, with audit trails, on behalf of clinicians who have explicitly delegated them.
The role of the physician moves from operator to author and reviewer. The chart becomes a consequence of care, not its bottleneck.
The next generation of clinical software is not better forms. It is fewer of them.
What “agentic” actually looks like
Listens. Retrieves. Reasons. Acts.
One subacute knee pain visit, compressed. The clinician keeps the gaze, signs at the end. The chart, the orders, and the referral are consequences, not prerequisites.
- Listens⋯
- Retrieves⋯
- Reasons⋯
- Acts⋯
illustrative · scripted · all four artifacts presented to the clinician for review, not auto-filed
Five principles
What we believe, in order.
- 01The physician is the user. Not the chart.
- 02Documentation is exhaust. Not work.
- 03Agents act, then explain. Not the reverse.
- 04Interop is a verb performed by software. Not a committee.
- 05Time at bedside is the only metric that matters.
The numbers
Half of every clinic hour. Four thousand clicks a shift. Most physicians, burned out. Cited.
Witness
If you’re a physician, count yourself.
One click is the only ask. No name. No email. No follow-up. Just a number that says how many physicians have read this and let it stand.
A position
Let physicians practice medicine.
That is the test. Anything that gets in the way — ours, theirs, anyone’s — deserves to be replaced.